Professional support for services working with Avoidant Restrictive Food Intake Disorder (ARFID)
This page has been produced by the North East and North Cumbria (NENC) Provider Collaborative. It is therefore intended for the use of all clinical staff and/or professionals from all services within NENC who are working with children and young people (CYP) and/or adults with ARFID/suspected ARFID.
These pages contain resources and signposting to support your work. This includes your clinical work, as well as information to support ARFID service developments in your area and your own continuous professional development (CPD) and professional support needs.
-
What is ARFID?
Avoidant Restrictive Food Intake Disorder (ARFID) is a classified eating disorder diagnosis within both the DSM-V (2013) and ICD-11 (2022) diagnostic manuals.
ICD-11 describe ARFID as:
Avoidant-restrictive food intake disorder (ARFID) is characterised by avoidance or restriction of food intake that results in:- the intake of an insufficient quantity or variety of food to meet adequate energy or nutritional requirements that has resulted in significant weight loss, clinically significant nutritional deficiencies, dependence on oral nutritional supplements or tube feeding, or has otherwise negatively affected the physical health of the individual; or
- significant impairment in personal, family, social, educational, occupational or other important areas of functioning (e.g., due to avoidance or distress related to participating in social experiences involving eating). The pattern of eating behaviour is not motivated by preoccupation with body weight or shape. Restricted food intake and its effects on weight, other aspects of health, or functioning are not due to unavailability of food, not a manifestation of another medical condition (e.g. food allergies, hyperthyroidism) or mental disorder, and are not due to the effect of a substance or medication on the central nervous system including withdrawal effects.
The ICD-11 essential diagnostic criteria is defined as:
- Avoidance or restriction of food intake that results in either or both of the following:The intake of an insufficient quantity or variety of food to meet adequate energy or nutritional requirements that has resulted in significant weight loss, clinically significant nutritional deficiencies, dependence on oral nutritional supplements or tube feeding, or has otherwise negatively affected the physical health of the individual.
Significant impairment in personal, family, social, educational, occupational or other important areas of functioning (e.g., due to avoidance or distress related to participating in social experiences involving eating).
- The pattern of eating behaviour is not motivated by preoccupation with body weight or shape.
- Restricted food intake and consequent weight loss (or failure to gain weight), or other impact on physical health or related functional impairment, are not due to unavailability of food; are not a manifestation of another medical condition (e.g., food allergies, hyperthyroidism) or mental disorder; and are not due to the effects of a substance or medication, including withdrawal effects.
It is important to note that selective eating applies to almost all people and exists as a continuum, or a spectrum, from disliking a few foods to significant restriction and avoidance. ARFID is the clinically diagnosable and severe end of this spectrum. It is not ‘fussy eating’, and the eating restriction is such that it has a significant detrimental impact on the quality of life of those affected (and their families). ARFID does not occur exclusively in low-weight status, and it is important to recognise that significant nutritional deficiency can also occur in average, and above-average, weight individuals.
ARFID is commonly associated with co-morbid autism where the avoidance of foods often stems from sensory specificity. However, not all individuals with ARFID have autism and not all individuals with autism have ARFID. Individuals can present with a chronic history of food avoidance, such as long-term sensory specificity which has worsened to meet a clinical threshold over time.
They can also present with an acute onset of food avoidance such as a sudden restriction of foods secondary to phobia (e.g. vomiting, choking or contamination). This is often associated with trauma: however, this does not need to be a direct traumatic experience. For example, witnessing a choking episode may be sufficient to trigger the phobic avoidance.
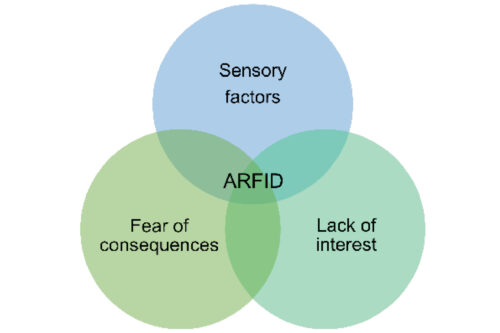
ARFID is often best understood as per the Venn diagram below. Most of the time, a person struggling with ARFID will have more than one presentation in combination.
-
I want to understand more about ARFID
If you’d like to understand more about ARFID you can view our co-produced NHS-England Film featuring both clinicians and a parent story here: NHS England ARFID Awareness Film
And the associated ARFID awareness leaflets here:
ARFID Parent Carer leaflet
Easy Read ARFID Parent Carer leafletDr Evie Bamingbade’s recent research update also provides an excellent, rich understanding of ARFID across presentations and diagnostic pathways, and has been shared with kind permission.
-
I’m setting up a service, are there any resources?
THE NENC ARFID Project has co-produced resources to support the development of local services.
This example of a CYPS Multi-Professional Mental Health Specialist ARFID Assessment Form can be used to inform and support your initial assessment process.
We have also co-developed an ARFID Severity Index and Severity Matrix tool for both children and adults with our national partners. These tools, and their support tools can support services in thinking about their acceptance criteria for both CYP and adults. The matrix tools are currently undergoing a proof-of-concept scoping validation research process.
Other national resources available include:
An extensive breadth of assessment tools are available from the Maudsley Centre for Child and Adolescent Eating Disorders under ‘ARFID assessment tools and resources’. These include short assessment screen tools which are helpful in triage, and PARDI questionnaire/clinical interview tools which are helpful in assessment and/or diagnosis.
*please note that training is advised before using the full PARDI-AR-Q interview schedule.Literature detailing example specialist pathway is available here: Towards an evidence-based out-patient care pathway for children and young people with avoidant restrictive food intake disorder
Willmott et al 2024 published an excellent scoping review of psychological interventions and outcomes for ARFID with a more accessible article style also shared.
The NHS England Eating Disorder Services for Children and Young People – national guidance is available online.
The national commissioning guidance for adults is available here: A Framework for Good Practice in Delivering Support for Adults and Older Adults with ARFID
-
I’m thinking of developing patient or carer groups, is there anything that could support this?
Group programmes are available across the country in a range of formats. These include:
- 2 parent group sessions for basic psycho-education and to assess readiness before starting 1:1 clinical work
- Clinical pathways with the offer being parents groups (face to face). In some places, these are ‘symptom based’ and without formalised or diagnostic assessment
- Adjunct or supplementary support groups and drop-in formats
- Peer support formats
- 3rd sector carers groups programmes
- 3rd sector ARFID group programmes (for adults / those over 16)
Group programme offers also vary in terms of their number of sessions, duration and capacity. Content also varies but they all typically include psychoeducation, with longer group programmes including more details on developing effective carers or treatment/exposure strategies.
Various group-based studies are emerging to help close the research gap in this area. These include a 2020 pilot trial of SPACE-ARFID (a novel parent based programme) and a Brief report into early intervention in children with ARFID/ARFID-like symptoms (2025). Group programme research is emerging all the time tentatively showing positive outcomes both for nutritional change and patient/carer experience. Group programmes appear to show tentative capability for managing high volumes of need in a cost-effective way, particularly for those with mild to moderate presentations, or in younger ages.
Whilst robust evidence is emerging, speaking with clinicians who have or do run programmes, for their insights and reflections can be helpful. Hazel is an Occupation Therapist working with South Yorkshire Eating Disorders Association (SYEDA). SYEDA are a 3rd sector organisation running an effective ARFID group programme for 16-24 year olds. She has kindly shared her main reflections on what makes this group successful:
- Start with the person at the centre – this is their journey
- Everyone is different. Therefore, make the group programme focused on individual goals – weave opportunities for individuals to develop, build and reflect on this as often as possible.
- Offer a safe group space to reflect, explore and understand eating difference
- Remove as many rules as possible (e.g. what people have to ‘complete’ or how they should interact)
- Ensure your participation numbers enable everyone to feel heard and to be validated
- Create a group for people to ‘come as they are’
- Clinician skill is more than just ARFID knowledge – it’s about hearing people’s stories and being able to pick out what is important.
-
I’m setting up a service, are there any networks?
The NENC CYP Provider Collaborative ARFID Project links ARFID developments as part of various eating disorder and service improvement workstreams. If you would like to find out more information about either group, please contact: [email protected]
The NENC also holds an extensive contact/distribution list for the sharing of updates, resources and training opportunities. If you wish to be included on these distribution lists, please contact the ARFID Project support officer: [email protected] letting her know where your service is based, and which age range you are interested in hearing about.
-
Where can I find examples of other ARFID services?
The North East and Yorkshire Regional Mental Health Team FutureNHS Platform contains a significant amount of recorded content and examples of other services from North East and Yorkshire Regional Mental Health Team
To access this, register on the FutureNHS Collaboration Platform
Then request access to the North East and Yorkshire Regional Mental Health Team
Once permission is granted, follow this path by clicking each tab on the website in turn:
- Childrens and young peoples mental health
- Eating disorders
- ARFID
- Service showcase
These FutureNHS pages also contain ARFID data mapping reports from across the region.
Please note: this content is from CYP services however many of the principles are applicable across the ages.
-
What have service users and families told us they want from professionals?
The NENC ARFID Project has co-worked with many people with lived experience of ARFID, and their families. It is incredibly important to them that that the professionals they see:
- Listen and take their concerns and worries seriously so that they feel heard and understood
- Act with empathy and compassion for the challenging situation they are in
- Are non-judgemental, non-critical and non-blaming
- Avoid making assumptions
- Make reasonable adjustments to accommodate their needs and communication preferences – this is particularly important for those with co-occurring autism
- Take reasonable steps to improve their knowledge of ARFID or can appropriately acknowledge the limitations in their understanding and seek to signpost to those with more knowledge of the condition
In 2023 we also conducted a scoping survey within our region to explore the top priorities of families for any new and developing ARFID service or pathway. The top 4 priorities from those with lived experience were:
- That services create pathways which are clear and easy to navigate/understand. They wanted service users to avoid being ‘bounced around’ different services
- That clinicians/professionals have adequate knowledge and skills to support them and their loved ones
- That service users are seen quickly from the point of referral (defined as within 4 weeks for routine referrals/within 1 week for urgent referrals)
- That services seek to include clear and comprehensive ARFID diagnosis if/where possible
-
Where do I go for Continued Professional Development (CPD?)
The North East and Yorkshire Regional Mental Health Team FutureNHS Platform contains a significant amount of recorded CPD content*
To access this, register on the FutureNHS Collaboration Platform
Then request access to the North East and Yorkshire Regional Mental Health Team
Once permission is granted, follow this path by clicking each tab on the website in turn:
- Childrens and young peoples mental health
- Eating disorders
- ARFID
- Training
Amongst others, the content includes 1 hour training modules* on:
- ARFID early identification training
- Assessment, diagnosis and identification of risk
- Nutritional strategies for ARFID
- Paediatric management of ARFID
- ARFID treatment options
- Managing emetophobia and choking phobia in ARFID
- Family Based Treatment in ARFID
* Please note: this content is from CYP perspective however many of the principles are applicable across the ages.
Through the North East and Yorkshire Regional Mental Health Team Future NHS pages you will also find:
- National webinars on all-age services and delivering support to adults and older adults
- A 3-hour introduction to ARFID training module
- A 1-hour learning event on communication and language for working with autist people
- Training on autism and eating disorders
Training on how to use CCi guided self-help worksheets - Motivational interviewing training
You can also find course-style learning material from: www.bebodypositive.org.uk under the ARFID and clinician tabs.
The National Centre for Autism and Mental Health runs a 3-day online training course for Autism and Eating Disorders
Although the content was only validated until 13th December 2026, two dietetic professors have developed and shared a free CPD learning module on the fundamentals of malnutrition in children
-
Are there any learning and development opportunities locally?
The North East and Yorkshire Regional Mental Health Team are running an ARFID Champions programme (for professionals working with CYP across our region). To find out more, please contact [email protected]
The North East and Yorkshire Regional Mental Health Team are running an ARFID Champions programme (for professionals working with CYP across our region). To find out more, please contact: [email protected])
Eating Distress North East (EDNE) deliver a range of CPD-accredited education and training sessions on eating distress/disorders. Focused on increasing knowledge, understanding and confidence, they promote early identification, intervention and recovery. All our education and training services are informed and underpinned by our extensive experience supporting people with eating distress:
- Working with eating disorders for professionals – This training assists professionals with early identification of an eating disorder /eating distress, builds confidence and explores strategies to best support those in their care.
- Understanding Avoidant Restrictive Food Intake Disorder (ARFID) – Exploring misconceptions around eating disorders, this training develops an understanding of signs and symptoms and how to talk to someone about ARFID.
- Neurodiversity and eating distress – This training explores the links between neurodiversity and eating distress and supports participants to apply new knowledge effectively within their work setting.
- Supporting a work colleague – This training will help you to champion wellbeing and mental health in the workplace. You’ll learn about eating disorders and distress and how to apply this knowledge with care, compassion, and empathy for colleagues/employees impacted by it.
To find out more about EDNE’s training offers please email their Education and Training officer, Sarah Lou Murray at [email protected]
-
Are there any discipline specific resources?
The British Dietetic Association (BDA) has an ARFID Sub Group. This group is open to all dietitians and student dietitians for free if they are an existing member of the BDA and either the Mental Health Sub-Group or the Paediatric Sub-Group. The BDA ARFID sub-group hosts a CPD meeting every 2 months and has website pages full of relevant resources and signposting. Members only resources include competency standards for dietitians, an ARFID Dietetic Toolkit and food frequency sheets. The BDA ARFID Sub Group has also developed an ARFID study day and an ARFID Nutrition and Dietetic Resource (NDR). For details and to join please visit: ARFID Specialist Sub-Group – British Dietetic Association (BDA). You can also follow the subgroup on instagram via: @bda_arfidsubgroup
The award winning CYP ARFID position statement for dietitians is available here: ARFID Position Statement and will be reviewed and updated in 2026 to become an all-age position statement.
There is an informal WhatsApp group for occupational therapists (OT’s) working in eating disorders with an interest in ARFID. This group aims to connect and share resources, training, CPD, jobs or news stories. It is a semi closed group for only registered OT’s or OT students. Details of bi-monthly MS TEAMS CPD meetings are shared via this WhatsApp group. These meetings give further opportunity for networking and sharing resources. It is hoped that in time workstreams will be developed to enhance OT work and the evidence base for OT’s working with ARFID. The group is supported by North East and Yorkshire regional mental health team (NHS England) but OT’s are welcome from any part of the country. More information can be found from [email protected] or [email protected] or please use this QR code to request to join.
if you are aware of any additional discipline specific support networks that may be able to support and help others, please do let us know by emailing the ARFID project lead: [email protected]
-
Is there anything specific to primary care?
The British Dietetic Association ARFID Sub-Group wrote an awareness raising article – What is avoidant restrictive food intake disorder? – for the British Journal of GP’s Life Magazine which includes additional signposting information for primary care.
The Primary Care Children and Young People’s (CYP) Eating Disorders (ED) Decision Treehas been developed by North East and Yorkshire Regional Mental Health Team, in collaboration with their ED and Primary Care Clinical Leads, and the North East and North Cumbria Provider Collaborative. The tool explores what steps to take in primary care when a young person presents with restricted oral intake, and provides signposting information. The tool includes a blank page at the end for recording local service details.*
Pedi R-Mapp offers a structured approach to completing nutrition focused consultations for GP’s, nurses, health visitors, physiotherapists, paediatricians and school nurses. It may therefore support in the guided assessment of those with ARFID/restricted intakes though sensitive and specific nutritional and associated risk management should come from a registered dietitian.
As a national supervision initiative, BEAT host an Eating Disorders Community of Practice for nurses, GP’s and the primary care workforce. For more info visit their website.
*NOTE: text can be added to PDF documents using a PDF editor.
-
Are there any resources to support my clinical practice?
There are several resources that can be used to support professional and clinical practice:
-
- A collective of specialist dietitians from the BDA ARFID sub-group have co-produced a practical and helpful resource to support vitamin and mineral supplementation in those with ARFID or sensory difficulties (all age). And a blank template for adding your own frequently used preparations. These tools will be updated in 2026.
- Feeding and Eating Difficulties: guideline for assessment and management was developed in 2025 as part of the Paediatric Feeding Disorder (PFD) Community of Practice Steering Panel, led by Natalie Morris from The Feeding Trust, with contributions from the BDA ARFID Sub-Group Committee. It provides an assessment and management structure for understanding PFD Vs. ARFID presentations.
- The Dietetic Safe Discharge Letter Template for CYPS and Dietetic Safe Discharge Letter Template for Adults have been created by the BDA ARFID Sub-Group committee to support safe dietetic discharge, particularly where there is an assessment but no treatment pathway. They are designed to be lifted and used within local services and edited to meet your purpose.
- Several professional resources are available from ARFID Awareness UK
- Cognitive-Behavioural Therapy for Avoidant/Restrictive Food Intake Disorder: Children, Adolescents, and Adults (Book) by Jennifer J Thomas and Kamryn T. Eddy (available in print)
- CBT for ARFID: Patient and Family Workbook A guided self help guide for patients and families using CBT-ARFID (CBT-AR).
- And here you will find a 1 hour CBT-AR Training video for ARFID
- MEED Guidance for assessing and managing medical risks in eating disorders is the essential risk assessment tool used for all eating disorders, including ARFID, across all ages.
As well as supporting service development, the CYP ARFID Severity Matrix
Adult ARFID Severity Matrix, and support tools can be used to understand clinical severities and support the understanding of clinical priorities.- In partnership with other regional and national services, the NENC ARFID project also developed Emergency re-feeding plans for sensory restrictive eating disorder admissions to acute paediatric wards. This is suitable for all ages and was shared nationally. An additional patient-facing supplementary sensory admissions resource has been co-produced with wider services and service users.
- Pedi R-Mapp offers a structured approach to completing nutrition focused consultations for GP’s, nurses, health visitors, physiotherapists, paediatricians and school nurses. It may therefore support in the guided assessment of those with ARFID/restricted intakes though sensitive and specific nutritional and associated risk management should come from a registered dietitian.
- The ARFID Nutrition and Dietetic Resource (NDR) has been produced by a cohort of expert dietitians and is available to purchase.
- The Nutricia ARFID resource is an excellent introductory resource for professionals
- Clinical Considerations for Gastrostomy Feeding in Individuals with ARFID This paper was led by the NENC ARFID Project Lead together with committee members from the BDA ARFID sub-group, Parenteral and Enteral Nutrition Group (PENG), Learning Disabilities Sub-Group, Autism Sub-Group, Paediatric Sub-Group, with experts from Great Ormond Street Feeding and Eating Disorders Service, and by gaining legal expertise from a professor of medical law. The piece also heavily integrates the voices of those with lived experience through sharing case-studies and reviewing the work. The work examines the potential therapeutic role of gastrostomy feeding in those with ARFID, explores the clinical considerations and considers how this may reduce risks for some individuals
*NOTE: PDF documents may not be suitable for assistive technology. If you use assistive technology (such as a screen reader) and need a version of this document in a more accessible format, please email [email protected]
-
-
Are there any outcome measure tools?
As well as providing various validated assessment tools, the Maudsley Centre for Child and Adolescent Eating Disorders shares several downloadable resources. These resources include:
- ‘What matters to me’ parent/carers evaluations
- ‘ARFID Intervention Monitoring Sheet (AIMS)’ (parent/carers or self).
These tools can help you to evaluate clinical interventions and can support you in establishing meaningful shared clinical goals with service users.
-
What about supervision for my complex cases?
The offers below are currently only available for CYP services in the NENC region.
Between 2023 and 2025 the NENC CYP ARFID Project hosted an innovative Virtual Consultation Support (VCS) Pod monthly meeting for a 1.5 hour duration. This drew together a panel of regional expertise to facilitate remote consultation to all sectors and care services and all relevant professionals within NENC are also able to join as a CPD and learning exercise.
During operation, the ARFID VCS Pod supported 57 clinical cases, over 19 months, and provided a learning forum for countless others. Evaluations demonstrated that 100% of attendees would recommend the pod and it fulfilled 100% of attendees’ objectives. 97% agreed/strongly agreed that it was a safe place to ask questions, 74% learned a lot (26% learned a little) and 100% of attendees reported gaining practical ideas to clinically support families in our area.
Despite its success, the Pod was stood-down due to a lack of ongoing engagement and need. In response to this, Clinicians from our area can continue to access a similar format from the North East and Yorkshire Regional Mental Health Team. They offer a Community of Practice case consultation model where case examples from anywhere across the NEY region are discussed with practice suggestions shared by all joining members.
To join the Community or Practice or find out more please contact: [email protected]
-
Where can I learn more about Autism?
The National Centre for Autism and Mental Health has a range of courses for healthcare professionals ranging from short courses, to PG-Cert and PG-Dip higher education levels
This picky and selective eating affirmations resource is also really helpful for professionals to hold in mind. It comes from www.livedexperienceeducator.com which hosts a lot of valuable content related to neurodiversity.
The new professional developments for disordered eating website also contains developments and resources regarding neurodivergent affirming care.
-
What are the key national publications?
Current key national guidelines and publications include:
- ARFID Position Statement – BDA
- NHS England – Eating disorder services for children and young people: National guidance
- A Framework for Good Practice in Delivering Support for Adults and Older Adults with ARFID (NHS England)
- Medical Emergencies in Eating Disorders (RCP, 2022)
- Prevention of Future Deaths Reports (for Alfie Nicholls, Owen Hinds and Joshua Allcock)
-
Is there more information for patients and families?
There is a comprehensive website available with resources, webinar content and extensive signposting for patients of all ages and/or their loved ones.
Please direct patients and/or carers to Support for Avoidant Restrictive Food Intake Disorder (ARFID)
-
Where can I signpost patients to locally?
Service access for both assessment and treatment varies across NENC depending on age and locality. In most cases, dedicated ARFID services remain under development in local areas. Information about dedicated local pathways will be added as and when this is available
-
Website validity information
This page was reviewed by Clare Ellison (ARFID Project Lead) in February 2026.
Updates are added as relevant and appropriate, however the full content is next due for comprehensive review in February 2027.

