Our Model of Care and Support Spring 2026 progress update
Welcome to the spring 2026 programme update report, which summarises the key areas of work and progress we are making against the Model of Care changes we are implementing across the Trust.
Model of Care Programme – Update
In 2024, we launched a new intranet section about our Model of Care. This is the second Model of Care and Support programme update. Below, you’ll find the latest updates on progress we are making to implement our new Model of Care across the Trust.
If you have any questions about this work, or would like to be involved, please get in touch: [email protected]
As part of delivering our Trust Strategy and Model of Care, we have published our Service Change Plan, outlining the key improvements that will enable us to achieve this. Find out more about this here.
Model of Care Programme – Key highlights
- The NHS ten-year plan outlines a clear vision for neighbourhood health, and we are working with partners to progress hubs and new ways of working through a joined-up, person-centred approach.
- The Trust is shifting away from the traditional Care Programme Approach (CPA) and moving toward a new personalised care model. Training needs assessment and workforce planning approaches are underway, including a focus on developing clinical skills and supervision. This will support improved access to psychological therapies and other treatments for our patients.
- We are developing an intensive approach to supporting individuals in the community with the most complex mental health needs, working collaboratively with partners to support over 400 identified patients in this cohort.
- Business cases have been developed as part of a potential funded bid for MHEDs (Mental Health Emergency Departments), in Newcastle, Sunderland and Carlisle, aligned with the new 10-year NHS plan.
- Our inpatient provision is being redeveloped. We have updated the Adult Acute provision at Carleton Clinic, and Adult inpatients in Central, with Older People’s inpatients moving into the redeveloped inpatient accommodation at the St Nicholas site is now complete.
The Trust has a Model of Care Programme Board which meets monthly and receives progress update reports from the following sub-groups:
- Understanding you and helping you stay well
- Community treatment
- Serious mental illness & long-term complex needs
- Urgent care and crisis
- Inpatient care
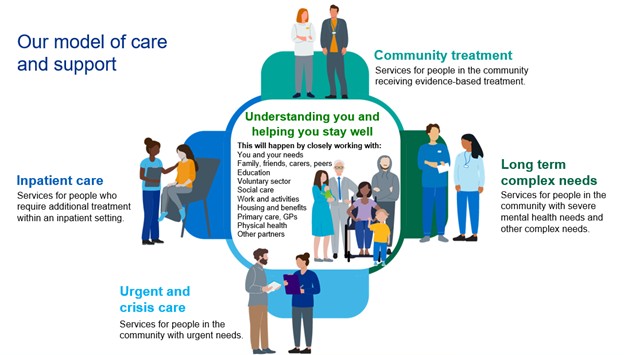
Understanding you and helping you stay well
If you have any further questions about this area of work, please contact our lead Chloe Mann via this email address: careandsupportprogramme@cntw.nhs.uk
Neurodevelopmental pathway
Some of the most challenged pathways for access to care and treatment are the waits for ADHD and autism assessment and diagnosis.
The Trust is working with neighbouring mental health trusts to continue the significant work underway to improve neurodevelopmental pathways. Together, we are planning to implement a better pathway across our partner organisations for people requiring ADHD and autism assessment and diagnosis.
This regional improvement work is happening alongside internal improvement planning led by these teams.
Launch of neurodiversity and emotional wellbeing service – North Cumbria Locality
A neurodiversity and emotional wellbeing service has launched in North Cumbria. This is a collaboration with system partners to ensure early help for young people under the age of 18 years.
Neighbourhood health
We are committed to working with partners across physical and mental health and social care in each local area, supporting submissions to the National Neighbourhood Health Implementation Programme, and aiming to be part of the first national cohort.
The NHS ten-year plan outlines a clear vision for neighbourhood health, and we are working with partners across all our places in their plans to take this forward.
Our clinicians are supporting several neighbourhood services for Mental Health and Wellbeing, including drop-ins, safe havens, and multi-disciplinary team working. These services are led by or delivered in partnership with GP practices, voluntary and community sector organisations (VCSE), CNTW, local government, and other stakeholders.
Some of our staff continue to support the development of a range of walk-in hubs in each area, which will transform how people access care within their communities.
`United Newcastle – A Canny City`
Building on the success of ‘The Space’ Hub in Newcastle, there will be a city wide roll out in 2026 to extend the coverage of hubs in Newcastle under the title of `United Newcastle, A Canny City`, extending the offer to a further three hubs.
Two sites have been identified for Blakelaw and Throckley. There are really positive relationships with Newcastle University, who are also wanting to have a hub specifically for their students within the university campus, making this the third new hub.
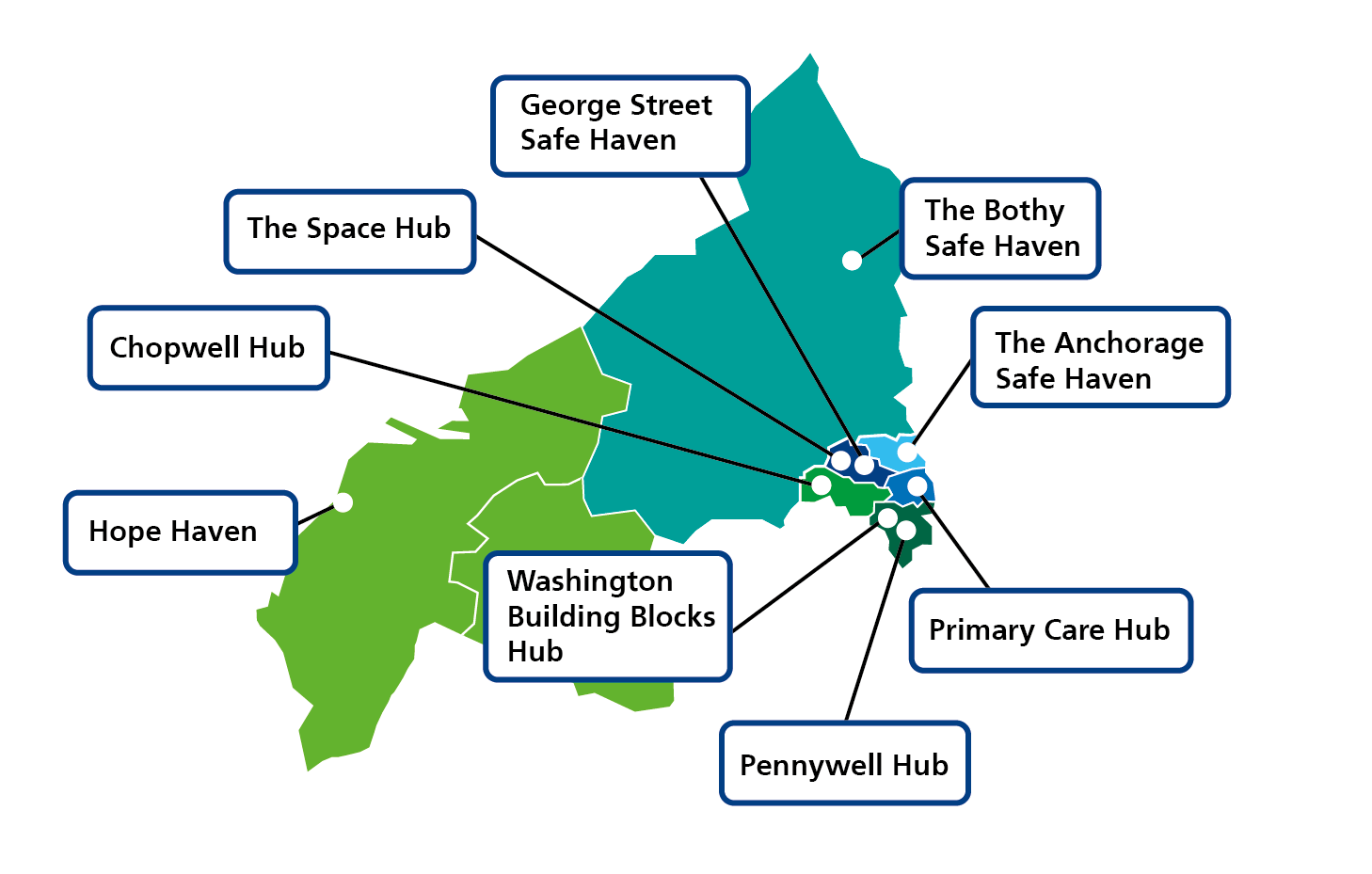
Hubs
- The Space Hub – Cruddas Park, Newcastle West
Lead provider – Co-produced CNTWPCN. Opened February 2024
Evaluation – ICB - George Street Safe Haven – Newcastle
Lead provider – Everyturn. Opened January 2025
Evaluation – Everyturn and TIG - The Bothy Safe Haven – Ashington, Northumberland
Lead provider – Everyturn. Opened March 2024
Evaluation – Everyturn and TIG - The Anchorage Safe Haven – Wallsend, North Tyneside
Lead provider – Everyturn. Opened July 2025
Evaluation – Everyturn and TIG - Primary Care Hub – South Tyneside
Lead provider – Primary Care. Opened 2022
Evaluation – ICB - Washington Building Blocks Hub – Washington, Sunderland
Lead provider – ICB Initiative. Opened March 2025
Evaluation – ICB - Pennywell Hub – Pennywell, Sunderland
Lead provider – ICB Initiative. Opened March 2025
Evaluation – ICB - Hope Haven – Copeland, North Cumbria
Lead provider – Co-produced. Opened Autumn 2025
Evaluation – Ipsos on behalf of national programme partners - Chopwell Hub – Chopwell, Gateshead
Lead provider: Co-produced. Opened July 2025
Evaluation: ICB
The Hope Haven 24/7 neighbourhood mental health care model national pilot
Since the last update, Hope Haven has now gone live with all aspects of its proposed offer (see next page). Refurbishment of the building on King Street (Whitehaven) is now complete and we are delivering the service from this venue in the town centre.
To date, Hope Haven has delivered walk-in, virtual and outreach appointments to over 1000 people so far.
We have also gone live with a single patient record system across all 6 partners working into the Hope Haven, allowing a quicker and more transparent working model across the system.
Person in need
Hope Haven
- Open access space designed to promote integrated working.
- Bookable rooms and group spaces.
- Hub/spoke delivery model for outreach to rural communities.
- Community owned.
- Recovery Cafe / out of hours service.
Person in need accesses support best aligned with their presenting needs – step up/step down
Trusted Conversations
Short stay beds (Home Group)
- 4 short stay beds with 24/7 access to support.
- Length of stay determined by need.
- Open access – Gender inclusive step up/step down support.
Inpatient beds (CNTW)
- Urgent Inpatient Care.
- Formal Admission – step up from short stay beds or community.
- Providing wider system integration.
Holistic Mental Healthcare
Specialist clinical intervention and oversight
Non clinical care manager mental health (Everyturn)
- Distress brief intervention.
- Together in a crisis.
- Hospital discharge.
Whole person wellbeing support (Home Group)
- Programme of wellbeing groups.
- Open access.
- Facilitated at Hope Haven and spoke sites.
Wider determinates of health supported by system partners
- iCan Wellbeing Group CIO
- Whitehaven Community Trust Ltd
- Cumbria Health
- The Well
Recovery
Relapse prevention/wellbeing maintenance
- Increased recovery capital.
- Community based support network.
- Peer support.
- Warm handover: Social Care, Primary Care etc.
Offer overview
Wellbeing Hub and Community Outreach
Individual Support
- Mon-Fri 9.30am-12midnight (walk-in, telephone, online access).
- Sat-Sun 4.00pm-12midnight (walk-in, telephone, online access).
Wellbeing hub/groups
- Facilitated customer led activities in hub
- Facilitated activities in spoke sites and other community settings.
- Integrated working in hub.
- Wheels of Wellness.
Community outreach
- Distress Brief Intervention (DBI).
- Together in a Crisis (TIAC).
- Hospital discharge.
Short Stay Beds
- 4 community-based beds with 24/7 support.
- Office and therapeutic space for crisis teams – 24/7 access.
- Short term stay 48-72 hours.
Collaborative MDT – Health, Social Care and VCSE
We have recently submitted bids for national funding to create more Neighbourhood Mental Health Centres, building on the Hope Haven model, in Carlisle, Northumberland, Newcastle and Sunderland. We will share more about these plans soon.
Read more about these national Neighbourhood Mental Health Hub Pilots.
Community Treatment
If you have any further questions about this area of work, please contact our lead Anna English via this email address: careandsupportprogramme@cntw.nhs.uk
Outcome measures for patients
The Trust is strengthening its approach to paired outcome measures which track progress before, during and after care. These include both Patient Reported Outcome Measures (PROMS) and Clinician Reported Outcome Measures (CROMS), developed in line with national guidance. Through dashboard developments within the Trust, clinicians can view the progress of individuals.
Since national measures for Carer Reported Experience aren’t widely available, there’s an opportunity to develop a local version that reflects carers’ perspectives accurately.
NHS England has recently launched a national PROMs dashboard where the use of PROMs by NHS provider Mental Health Trusts is followed. This work is supported by a regional community of practice facilitated by NHS England, which CNTW updates and feeds back into.
Changing our approach to care
The Trust is moving away from the traditional Care Programme Approach (CPA) and toward a more personalised care model, with a strengthened role for the multi-disciplinary team in overseeing care management and managing risk.
Depending on the complexity of an individual’s needs, service users may be supported by a named worker from another organisation, such as a housing provider or social worker.
Changes have been piloted in Keswick and Solway, and North Northumberland, which have been evaluated with a view to expanding the approach to the wider Trust. These pilots tested new ways of working to provide a more personalised approach to meet the service user’s needs by utilising multi-discipline meetings to assess these needs in all aspects of life.
Policies and guidance are currently being updated to reflect and support the change, as well as capturing any further developments to national policy regarding changes to CPA.
Changing our approach to delivering care – including expanding Psychological Therapies and other treatment options
A training needs assessment and psychology workforce plan are in development, with the next phase focusing on developing clinical skills and supervision.
This is in parallel to wider workforce planning related to moving away from Care Programme Approach, with opportunities to upskill staff and expand the range of evidence-based treatments offered to all ages and across pathways, and to ensure our clinicians are focussed on activities which have the most positive impact.
Clinical Reported Outcome Measures & Diagnosis Recording
The Trust is developing plans to focus on the use of a nationally recommended Clinical Reported Outcome Measure (CROM) tool, in order to support a standardised care management approach across adult CTTs in the first instance.
Further information regarding the tool’s use, training of staff, and rollout to wider services will be shared in future communications.
In parallel, communications have been shared with staff regarding improving rates of diagnosis recording in RiO, as a fundamental part of assessing needs.
Improving transitions between child and adult pathways
An ongoing piece of work is underway looking at transitions between children’s and adult pathways across the Trust to ensure these are as seamless and timely as possible.
By better identifying transition points in a service user’s pathway, we can improve how this transition happens through use of ‘Moving on’ plans, forward referral criteria and making transition to the relevant service a goal from the outset.
Further information will be communicated in future updates.
Long Term Complex Needs
If you have any further questions about this area of work, please contact our lead Anna English via this email address: [email protected]
Intensive case management
The Trust is developing a more assertive approach to supporting patients with serious mental health needs in the community, working closely with partners.
Over 400 patients were identified using key criteria such as missed appointments or medication, with clinicians reviewing caseloads to ensure no-one has been missed. Following work between operational and digital colleagues to provide a digital solution to support the identification and review of those who may benefit from this approach, we now have a digital solution in place.
A new model is being developed to manage the care of these individuals proactively, safely and effectively in the community, while existing care and risk management plans are being reviewed to ensure safety in the short term.
Rehabilitation pathways
Community caseloads have also been reviewed to identify service users who may benefit from a refreshed approach to rehabilitation pathways. This work is in partnership with inpatient services, who are reviewing their models of care.
The Trust is engaging with the ICB and Tees, Esk & Wear Valley NHS Trust to look at the regional rehabilitation offer, to ensure a consistent offer across providers.
Community Clozapine (antipsychotic medication) clinic
Phase one of expanding the community-based Clozapine service is complete, with staff recruited and the new clinic building open and functioning.
This service went live in April 2026
This will allow more people to access Clozapine in a safe, controlled environment without needing to be admitted to hospital — helping reduce distress and improve access to care, while reducing pressures on beds.
Urgent Care and Crisis
If you have any further questions about this area of work, please contact our lead Chloe Mann via this email address: [email protected]
NHS 111
The Trust delivers the Mental Health aspect of the 111 service via its Initial Response Service (IRS) call centre based in Sunderland. This model is now fully live across the Trust, supporting consistent and accessible mental health care, strong integration with local partners and the Trust’s Crisis teams. Impact evaluation including demand on the service is ongoing.
Supporting those frequently admitted
The Trust is reviewing service users with repeated inpatient admissions to understand their needs more clearly.
A new community-based support forum has been developed for those identified, to help reduce re-admissions, and to offer more effective ongoing care for those who frequently access emergency care and urgent care services.
Mental Health Emergency Departments (MHEDs)
We have recently submitted bids for national funding to create ‘Mental Health Emergency Departments’ in Newcastle, Carlisle, and Sunderland, as part of a potential government funding bid for MHEDs. The aim is to ensure individuals experiencing mental health crisis are supported in dedicated, therapeutic space — reducing time spent in general Emergency Departments and ensuring access to specialist mental health care.
We will share more about these plans soon.
Read more about national plans for these centres here.
As well as this, work is progressing with acute and third sector colleagues on improving access to urgent care for mental health patients, and a review of crisis pathways.
Hospital to Home (H2H)
A new discharge model has been designed to ensure patient’s needs and individual circumstances are fully understood before leaving hospital.
Daily collaborative meetings bring together all relevant professionals to plan safe, appropriate discharge destinations.
This ensures patients aren’t kept in clinical environments longer than necessary, supporting better recovery outcomes.
H2H launched in November 2025, with each locality now having a dedicated resource including bed management, discharge facilitators and social work, working together to remove barriers for those clinically ready to be discharged.
Two pathways one goal: safe support recovery
Early response/Prevention
Community Care and Treatment -> Admission -> Hospital admission when community care isn’t enough. A clear purpose of admission, can only be provided in a hospital -> Enhanced person-centred community care plan. Augmented CRHT, Step up/ increased social care -> Relapse indicators/increased risk, Amber Flag, Monitor at Flow Meeting.
Hospital to Home pathway
Discharge plan
Support begins at admission; planning starts day one. Hub coordinates all partners to unblock barriers. Focus on safe, timely discharge. Crisis Ready for Discharge – Next step care plan (amber). CTT ready for discharge (green) -> Community Care and Treatment.
Inpatient care
If you have any further questions about this area of work, please contact our lead Russell Patton via this email address: [email protected]
Central Re-Provision (Adult)
Transfer of adult services from the CAV to the St Nicholas site has completed. The Central S136 suite is being temporarily housed in Lamesley. Through the CEDAR Board, a lesson learned exercise was completed in November.
Central Re-Provision (Older Adult)
Two older adult wards will also transfer from CAV to the St Nicholas Hospital site. Refurbishment of two additional wards is underway. The planned move is expected to be May 2026.
Moving Inpatient care from Yewdale to Carleton Clinic
Following considerable engagement, and linked to the official opening of Hope Haven’s 4 ‘hospitality beds’, the Yewdale ward closed on 29 August 2025.
Learning Disability Bed Provision
The temporary closure commenced on 10 November 2025, following the appropriate discharge/transfer of remaining patients – Rose Lodge was already closed to new admissions.
This temporary closure is an opportunity for us to explore new ways to provide better support for people with learning disabilities.
Shift Pattern Review
The consultation period has now closed and feedback has been incorporated. New shift patterns are now live.
Enhanced Multi-disciplinary Team (EMDT)
The working age adult acute pathway continues to develop and embed the EMDT model which includes 7-day senior clinical leadership presence across the Inpatient Group.
Hospital to Home- H2H
As previously described H2H teams launched formally in November 2025. Performance is being monitored to measure both success and areas for improvement with the service. With the embedding of the service within working age and older people’s services, considerations are being given to the extension into rehab service.
Culture of Care Pilot Wards
Selected inpatient wards participated in a national pilot to embed learning from the Culture of Care Standards. These pioneering sites are spearheading change, with lessons and best practices being shared Trustwide with national guidance and support. The pilot completed at the end of March 2026.
Inpatient Quality Transformation Programme (IPQT)
The Trust is actively collaborating with regional partners and the ICB in the Inpatient Quality Transformation Programme, a strategic initiative focused on enhancing safety, effectiveness, and patient experience across all inpatient settings.
Culture of Care Pilot Wards
Selected inpatient wards participated in a national pilot to embed learning from the Culture of Care Standards. These pioneering sites are spearheading change, with lessons and best practices being shared Trustwide with national guidance and support. The pilot completed at the end of March 2026.
Read more about the culture of care standards for mental health inpatient services here.
